Diabetic Ketoacidosis (DKA) is a life-threatening complication of diabetes, primarily affecting Type 1 diabetics. Advanced treatments include IV fluids, insulin therapy, and electrolyte replacement. Emerging technologies like closed-loop insulin systems and BHB monitoring enhance management. Preventive strategies and regular monitoring are crucial for reducing DKA risks and improving outcomes.

Introduction:
Diabetic Ketoacidosis (DKA) is a serious and potentially life-threatening condition that primarily affects individuals with diabetes, particularly Type 1 diabetes. It occurs when the body starts breaking down fats too quickly due to a lack of insulin, leading to the production of ketones, which makes the blood acidic. Understanding the advanced treatments for DKA is crucial for effective management and prevention of complications. This guide will walk you through the key aspects of advanced DKA treatments, presented in an easy and understandable language.
Understanding Diabetic Ketoacidosis (DKA)
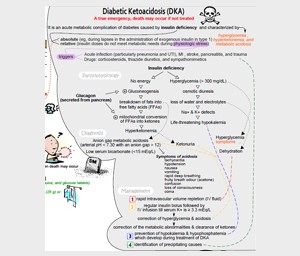
Before diving into treatments, it’s important to grasp what DKA is and why it occurs. In individuals with diabetes, especially those with Type 1 diabetes, the body either doesn’t produce enough insulin or doesn’t use it effectively. Insulin is essential for helping glucose (sugar) enter cells to be used for energy. Without sufficient insulin, the body starts breaking down fat as an alternative source of energy, leading to the production of ketones. When these ketones build up in the bloodstream, they make the blood acidic, resulting in DKA.
Symptoms of DKA
Recognizing the symptoms of DKA early can lead to prompt treatment and better outcomes. Common symptoms include:
If you or someone you know experiences these symptoms, seek medical attention immediately.
Advanced Treatments for DKA
Treating DKA requires a multi-faceted approach that addresses dehydration, insulin deficiency, and electrolyte imbalances. Here are the advanced treatments commonly used:
1. Intravenous (IV) Fluids
Purpose: To rehydrate the body and dilute the excess sugar in the blood.
Process: Patients are typically given IV fluids to replace lost fluids and electrolytes. The type and amount of fluid administered depend on the severity of dehydration and electrolyte imbalances. Normal saline is often used initially, followed by fluids containing glucose once blood sugar levels drop to prevent hypoglycemia.
2. Insulin Therapy
Purpose: To reduce blood sugar levels and halt the production of ketones.
Process: Insulin is administered intravenously to quickly lower blood glucose levels. The dosage is carefully monitored and adjusted based on frequent blood glucose and ketone measurements. Once blood sugar levels approach normal, a transition to subcutaneous insulin (injected under the skin) is made.
3. Electrolyte Replacement
Purpose: To correct imbalances of key electrolytes like potassium, sodium, and bicarbonate.
Process: Electrolytes are crucial for normal cell function, particularly heart and muscle cells. DKA often leads to low potassium levels, which can be life-threatening. Potassium is administered intravenously, with close monitoring of blood levels to avoid overcorrection. Other electrolytes, such as sodium and bicarbonate, are also monitored and adjusted as needed.
4. Monitoring and Supportive Care
Purpose: To ensure comprehensive management and address any complications that arise.
Process: Continuous monitoring of vital signs, blood glucose, ketone levels, and electrolytes is essential. This helps in adjusting treatments promptly. Additionally, supportive care may include oxygen therapy if breathing is compromised, and treatment for any underlying infections or illnesses that may have triggered DKA.
New and Emerging Treatments
Advancements in medical technology and pharmacology have led to the development of new treatments and management strategies for DKA:
1. Closed-Loop Insulin Delivery Systems (Artificial Pancreas)
Description: These systems continuously monitor blood glucose levels and automatically adjust insulin delivery.
Benefits: They provide tighter glucose control, reduce the risk of DKA, and can improve overall diabetes management.
2. Sodium-Glucose Cotransporter-2 (SGLT2) Inhibitors
Description: These are a class of medications that help lower blood sugar by causing the kidneys to remove glucose from the body through urine.
Benefits: While they are primarily used for managing Type 2 diabetes, they are being explored for their potential in preventing DKA in specific populations. However, they must be used cautiously as they can sometimes increase the risk of DKA.
3. Beta-Hydroxybutyrate (BHB) Monitoring
Description: BHB is a type of ketone body. Monitoring BHB levels in the blood can provide more accurate and timely information about ketone levels compared to traditional urine tests.
Benefits: Early detection of rising ketone levels can lead to prompt intervention and prevent the progression to DKA.
4. Continuous Subcutaneous Insulin Infusion (CSII)
Description: Also known as insulin pump therapy, CSII delivers insulin continuously through a small device worn on the body.
Benefits: It allows for more precise insulin dosing, better mimicking the body's natural insulin release, and can help prevent blood sugar fluctuations that may lead to DKA.
5. Telemedicine and Remote Monitoring
Description: Utilizing telemedicine platforms and remote monitoring devices to manage diabetes.
Benefits: Provides real-time monitoring and support from healthcare professionals, ensuring prompt intervention if blood glucose levels become dangerously high, thereby reducing the risk of DKA. This approach also improves patient education and adherence to treatment plans.
Preventing DKA
Prevention is always better than cure, especially for DKA. Here are some key preventive strategies:
Conclusion
Diabetic Ketoacidosis is a serious complication of diabetes that requires immediate medical attention. Advanced treatments for DKA focus on rehydration, insulin therapy, and correction of electrolyte imbalances. With new technologies and medications, the management of DKA continues to improve, offering better outcomes for patients. Preventive measures, such as regular monitoring and proper diabetes management, are crucial in reducing the risk of DKA. If you have diabetes, work closely with your healthcare team to develop a comprehensive plan to manage your condition and prevent complications like DKA.